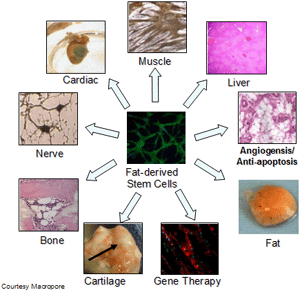
Sources of Equine Stem Cells
Adipose(Fat) Tissue
Adipose-derived stem cells are currently being utilized in the United States, and their application is commercially available through Vet-Stem. Vet-Stem, centered in San Diego, California, offers stem cell therapy for tendon and ligament injuries in horses and dogs. In order to harvest adipose cells, about two tablespoons of fatty tissue is taken from the dock, or top, of the horse’s tail under local anesthetic. If Vet-Stem is consulted, they provide the veterinarian with a collection kit where the sample can be stored in
refrigeration for its transportation to California. In a four hour process, the necessary cells are isolated through floatation and digestion, and then packed into pre-loaded syringes. No culture step is needed because of the number of cells naturally present. The entire process takes no more than forty-eight hours. Once the cells are returned to the veterinarian, the personalized dosage is injected into the injury site (Pincock 2005). The horse is then started on a carefully monitored exercise program. Adipose-derived stem cells have many advantages to their use. They are easily and non-invasively obtained with very little pain to the donor. Also, without a culture step, there is a shorter period between collection and implantation than other cell derivations, and the total cost is cheaper than that of the other currently available cell sources (Richardson et al. 2008). Adipose-derived cells provide not only enough cells for treatment without culturing, but enough cells are left over to freeze for later use if needed (Pincock 2005). A study done by Vet-Stem on 66 horses with a two-year follow-up after treatment of tendon injury showed a 77% return to prior level of performance and 94% were sound one year or more after treatment. In contrast, only 40-60% of horses with tendonitis treated with traditional therapies were determined sound one year after treatment (Vet-Stem 2005). The only major disadvantage in using these cells is that they are mesenchymal, meaning they only have the capacity to differentiate toward bone, tendon, ligament, and cartilage tissues. Cells with this limitation are called pluripotent. True stem cells are totipotent; they can become any cell type in the body. The restrictions on adipose-derived stem cells do not affect tendon regeneration, but could keep these cells from being useful for treatments involving other tissue types, such as organ tissues. However, for tendon injuries, adipose-derived stem cells seem to show promise. |
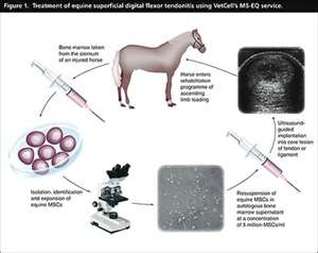
Bone Marrow
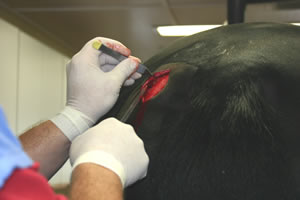
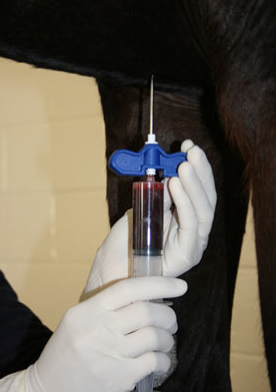
Most research studies have focused on the application and behavior of bone marrow-derived stem cells. In order to collect these cells, bone marrow is collected from the horse’s sternum under standing sedation (Pincock 2005). One of seven marrow spaces is isolated using ultrasound. Usually, spaces three through five are used
because they are the largest at up to five centimeters in diameter. About twenty milliliters of marrow is collected in syringes and sent to a lab for culture, due to the small percentage, 0.001-0.01%, of stem cells found in adult bone marrow (Fortier et al. 2011). In the lab, cells are isolated and then cultured to a minimum of ten million over a period of ten to thirty days, a much longer re-implantation period than adipose-derived cells (Pincock 2005). Implantation is then performed under tenoscopic guidance with general anesthesia (Smith et al. 2005). Like adipose-derived cells, bone marrow-derived cell services are commercially available. Through a company called VetCell, located in England, European and Australian consumers have access to stem cell treatments. VetCell offers training courses to veterinarians to allow them to learn about its technology, criteria for treatment, and practicalities. This could improve success rate of this company. VetCell claims that more than 400 horses have been treated as of 2008 with no adverse effects except for cosmetic needle tracts visible in ultrasound. Also, re-injury rates decreased from 56% to 18% in the same category of subjects when compared to conventional methods (Richardson et al. 2008). Another study showed a re-injury decrease to between 23% and 43% based on discipline (Smith 2008). A study on race horses with a two year follow-up stowed no adverse effects of the treatment with no aberrant tissue on histological examination. The re-injury rate of all racehorses with follow-up undergoing MSC treatment was 27.4% (Godwin et al. 2011). Dr. Lisa Fortier of Cornell University Veterinary School claims that “these cells [bone marrow-derived] have shown favorable affects on tissue organization, composition, and mechanics,” and are “easily and noninvasively obtained,” with a greater differentiation capacity than other mesenchymal stem cells, such as adipose-derived cells (Fortier et al. 2011). Despite this capacity, no bone or cartilage formation has been observed in post-treatment tendon (Smith 2008). In addition, horses are able to return to full training in 48 weeks, the rest period of conventional treatment (Smith et al. 2005). Like adipose-derived cells, these adult stem cells hold the possibility for autologous implantation, which would get rid of the issue of culture lag time (Richardson et al. 2008). Also, a study on rabbit tendon concluded that, in the rabbit, model stem cells do not lose their benefit as a tendon repair therapy option with aging even though the number of cells declines, and that stem cells can be cryogenically stored for 3 years and still effectively repair soft tissue injuries (Butler et al. 2005). This ability would further support the possibility of storing cells for autologous implantation for a long period of time. Despite all of this data to support bone marrow-derived stem cells, there are disadvantages to their use. The low number of stem cells in bone marrow leads to a long period between collection and implantation due to culture step (Richardson et al. 2008). This culture step also increases the price of this treatment over adipose-derived cells, and the cells have to be injected before fibroplasia forms, as longer periods between injury and treatment show lower success rates (Smith 2008). Like adipose-derived cells, these cells are mesenchymal and therefore have limited differentiation capacity, though they have been shown to differentiate more freely than adipose-derived cells. |
Fetal Tissue
Fetal-derived stem cells are a type of cell that is most commonly associated with the controversial human stem cell debate, because the fetus has to be aborted in order for the cells to be obtained. These cells are derived from blastocysts, which develop about one week after fertilization. The embryo forms around a cluster of cells known as the inner cell mass, which is where the fetal stem cells are found (Fortier 2003). Cells similar to these can be extracted from a 10 centimeter section of the umbilical cord, though it is unknown how different the properties of these cells are from actual fetal-derived cells (Pincock 2005). Fetal-derived cells have the ability to differentiate into any tissue type, meaning they are totipotent (Fortier 2003). These cells have only recently been included in stem cell research studies, so scientists are not as familiar with their properties as adipose and bone marrow-derived cells. According to Dr. Fortier of Cornell, “Most studies [until recent years] have focused on observance in culture,” (Fortier 2003). However, a new controlled study with fetal derived cells showed that tendons had significant structure improvement, were smaller, had smaller lesions with better fill, and had a greater return to a normal linear fiber pattern than placebo, or conventionally, treated tissue. Through experimentation over the past decade, the development of normal fiber pattern has been most closely linked to long-term success. Cosmetic needle tracts are also less visible after eight weeks with fetal-derived cell implantation than with bone-marrow derived cells (Watts et al. 2011). Still, the process used to obtain these cells involves the murder of an unborn fetus, followed by dissection of the spinal cord, brain, and heart tissues. It is therefore the most controversial of the cell linages, and would have trouble getting approval to be tested in humans.
|